WASHINGTON (AP) — Medicare recipients will get a premium reduction — but not until next year — reflecting what Health and Human Services Secretary Xavier Becerra said Friday was an overestimate in costs of covering an expensive and controversial new Alzheimer's drug.
Becerra’s statement said the 2022 premium should be adjusted downward but legal and operational hurdles prevented officials from doing that in the middle of the year. He did not say how much the premium would be adjusted.
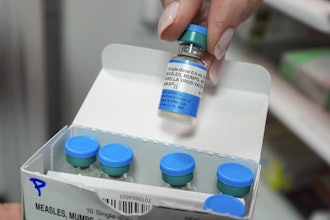
Medicare Part B premiums jumped by $22 a month, to $170.10, for 2022, in part because of the cost of the drug Aduhelm, which was approved despite weak evidence that it could slow the progression of Alzheimer's.
The Centers for Medicare and Medicaid Services has limited coverage of Aduhelm to use in clinical trials approved by the Food and Drug Administration or the National Institutes of Health. It began reassessing the premium increase under pressure by Congress and consumers.
The drug's manufacturer, Cambridge, Massachusetts-based Biogen, has cut the cost of the drug in half, to about $28,000 a year.
CMS cited the sharp reduction in the price of the drug and the limitations on coverage in concluding that cost savings could be passed on to Medicare beneficiaries. In a report to Becerra, the agency said the premium recommendation for 2022 would have been $160.40 a month had the price cut and the coverage determination both been in place when officials calculated the figure.
The premium for 2023 for Medicare's more than 56 million recipients will be announced in the fall.
“We had hoped to achieve this sooner, but CMS explains that the options to accomplish this would not be feasible," Becerra said. “CMS and HHS are committed to lowering health care costs — so we look forward to seeing this Medicare premium adjustment across the finish line to ensure seniors get their cost-savings in 2023.”