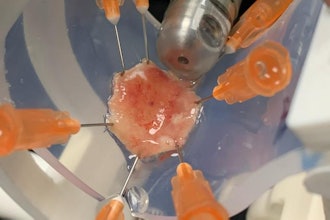
Scientists at The Hospital for Sick Children (SickKids) and the University of Toronto (U of T) have combined forces to develop a new approach to potentially treat tumor cells, called mechanical nanosurgery, even for aggressive, chemoresistant cancers.
Glioblastoma (GBM) is the most common and aggressive primary brain cancer. Despite various treatment options that exist, including surgery, radiotherapy, and chemotherapy, the median survival time for patients is only around 15 months.
The current global standard-of-care treatment for GBM patients includes chemotherapy using a drug called temozolomide (TMZ), which extends a person’s life expectancy by approximately two months compared to patients receiving radiotherapy alone. However, GBM cells can develop resistance to TMZ over time, reducing its efficacy and increasing the likelihood of tumor relapse.
In a study published in Science Advances, Dr. Xi Huang, a Senior Scientist in the Developmental & Stem Cell Biology program at SickKids, and Dr. Yu Sun, Professor of Mechanical Engineering and Director of the Robotics Institute at U of T, present a new approach to treat chemoresistant GBM using precision magnetic control in a process they call mechanical nanosurgery.
“Through the use of nanotechnology deep inside cancer cells, mechanical nanosurgery is a ‘Trojan Horse’ approach that could allow us to destroy tumor cells from within,” says Huang, whose previous research demonstrating that brain tumor cells are mechanosensitive helped to inform the approach. “By combining our expertise in biochemistry at SickKids and engineering at U of T, we’ve developed a potential new way to treat aggressive brain cancer.”
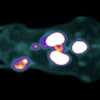
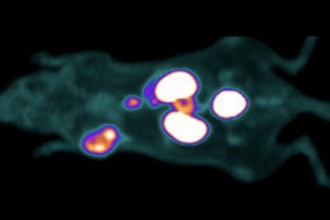
Developed with first author Dr. Xian Wang, current Assistant Professor at Queen’s University, former post-doctoral fellow in the Huang Lab and winner of a Lap-Chee Tsui Fellowship through the SickKids Research Training Centre, the mouse model used in the study showed that the mechanical nanosurgery process reduced GBM tumour size universally, including in TMZ-resistant GBM.
How mechanical nanosurgery works
Magnetic carbon nanotubes (mCNTs) are a form of nanomaterial – microscopic cylindrically-shaped tubes made of carbon and, in this case, filled with iron that becomes magnetized when activated by an external magnetic field. In the study, the research team coated mCNTs with an antibody that recognizes a specific protein associated with GBM tumor cells. Once injected into the tumor, the antibodies on the mCNTs cause them to seek out tumor cells and are absorbed by them.
“Once the nanotubes are inside the tumor cell, we use a rotating magnetic field to mechanically mobilize the nanotubes to provide mechanical stimulation,” says Sun. “The force exerted by the nanotubes damages cellular structures and cause tumor cell death.”
Exploring applications beyond brain cancer
Huang’s partnership with Sun at the U of T Department of Mechanical Engineering is continuing to build on the study findings. As their research continues, they note that mechanical nanosurgery may have further applications in other cancer types.
“Theoretically, by changing the antibody coating and redirecting nanotubes to the desired tumor site, we could potentially have a means to precisely destroy tumor cells in other cancers,” says Huang.