Researchers at the University of Houston are using glow-in-the-dark materials to enhance and improve rapid COVID-19 home tests. If you’ve taken an at-home COVID-19 or pregnancy test, then you’ve taken what is scientifically called a lateral flow assay (LFA) test, a diagnostic tool widely used because of its rapid results, low cost and ease of operation. When you read test results, you see colored lines.
“We are making those lines glow-in-the-dark so that they are more detectable, so the sensitivity of the test is better,” said Richard Willson, Huffington-Woestemeyer Professor of chemical and biomolecular engineering and professor of biochemical and biophysical sciences, who previously created a COVID smartphone-based app and test kit based on the technology underlying home pregnancy tests.
The first idea for glow-in-the-dark technology sprang from a star pasted on the ceiling of Willson's young daughter's bedroom. One night while he was putting her to sleep, he peered at the glow-in-the-dark star and his mind began to wander, applying its principles to science. Within days Willson and his team of students and postdocs was creating a test with glowing nanoparticles made of phosphors, which would make the particles even more detectable and the tests more accurate. Two of the students became the founders of Luminostics (now called Clip Health, a spinoff from the Willson lab).
Now in the Willson lab, the next generation is developing.
“In this new development, there are two tricks. First, we use enzymes, proteins that catalyze reactions, to drive reactions that emit light, like a firefly. Second, we attached those light-emitting enzymes onto harmless virus particles, along with antibodies that bind to COVID proteins,” reports Willson in the Royal Society of Chemistry’s journal Analyst.
The reason these steps are useful is that one antibody on a virus can bind to one COVID target on the test strip and bring along with it many light-emitting enzymes. So, the team gets more light for each target, thus needing fewer targets to see the light, making the test more sensitive.
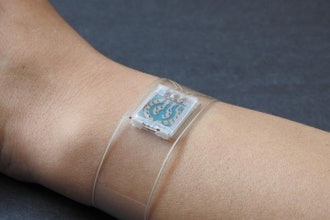
And while you might be able to read the results with your eye in a very dark room, the Willson team created a little plastic box to exclude light and let a smartphone camera do the reading.
“This is more reproducible and probably more sensitive, and with smartphones you can communicate the results to databases and things like that,” said the paper’s corresponding author Katerina Kourentzi, University of Houston research associate professor of chemical and biomolecular engineering. Jacinta Conrad, Frank M. Tiller Associate Professor of Chemical and Biomolecular Engineering, also from the William A. Brookshire Department of Chemical and Biomolecular Engineering at the University of Houston Cullen College of Engineering, is on team. Others from UH include the first author of the paper Maede Chabi, Binh Vu, Kristen Brosamer, Maxwell Smith and Dimple Chavan.
Willson adds the sensitivity is really excellent, better than essentially any commercial tests, making the technology useful in an array of medical arenas.
“This technology can be used for detecting all kinds of other things, including flu and HIV, but also Ebola and biodefense agents, and maybe toxins and environmental contaminants and pesticides in food,” said Willson.
So truly, the sky – and stars – are the limit.