Physician-scientists at Beth Israel Deaconess Medical Center (BIDMC) conducted a randomized controlled trial to determine whether virtual reality immersion can minimize the need for sedatives during hand surgery without negatively impacting patient satisfaction.
Common anesthesia practice for hand surgery combines a preoperative regional anesthetic and intraoperative monitored anesthesia care (MAC). Despite adequate regional anesthesia, patients may receive doses of intraoperative sedatives which can result in oversedation and potentially avoidable complications.
VR could prove to be a valuable tool for patients and providers by distracting the mind from processing noxious stimuli resulting in minimized sedative use and reduced risk of oversedation without negatively impacting patient satisfaction.
The hypothesis was that intraoperative VR use reduces sedative dosing during elective hand surgery without detracting from patient satisfaction as compared to a usual care control.
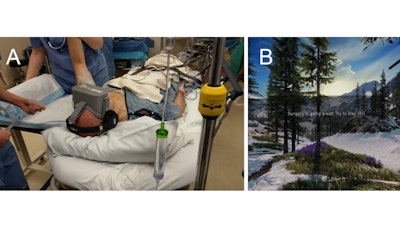
Forty adults undergoing hand surgery were randomized to receive either intraoperative VR in addition to MAC, or usual MAC. Patients in both groups received preoperative regional anesthesia at provider discretion.
Intraoperatively, the VR group viewed programming of their choice via a head-mounted display. The primary outcome was intraoperative propofol dose per hour (mg · hr-1). Secondary outcomes included patient reported pain and anxiety, overall satisfaction, functional outcome and post anesthesia care unit (PACU) length of stay (LOS).
Of the 40 enrolled patients, 34 completed the perioperative portion of the trial. VR group patients received significantly less propofol per hour than the control group (Mean (±SD): 125.3 (±296.0) vs 750.6 (±334.6) mg · hr-1, p<0.001).
There were no significant differences between groups in patient reported overall satisfaction, (0–100 scale, Median (IQR) 92 (77–100) vs 100 (100–100), VR vs control, p = 0.087).
There were no significant differences between groups in PACU pain scores, perioperative opioid analgesic dose, or in postoperative functional outcome. PACU LOS was significantly decreased in the VR group (53.0 (43.0–72.0) vs 75.0 (57.5–89.0) min, p = 0.018).
VR immersion during hand surgery led to significant reductions in intraoperative propofol dose and PACU LOS without negatively impacting key patient reported outcomes.