In a groundbreaking achievement, Oklahoma Children’s Hospital OU Health has performed the world’s first robotic Deep Brain Stimulation (DBS) procedure in a pediatric patient, resulting in immediate improvement in motor function the child did not have prior.
DBS, a surgical technique involving the implantation of electrodes into specific brain regions, has traditionally been used to treat movement disorders like Parkinson’s disease, essential tremor and dystonia. This procedure and the particular device have never been performed robotically in pediatric patients until now. The use of robotics enhances the surgical precision and safety of the procedure while also unlocking new possibilities for improved patient outcomes.
The medical collaboration with Bethany Children’s Health Center successfully rallied around 8-year-old Karleigh Fry, who has rapid-onset primary dystonia, a movement disorder that causes the muscles to react involuntarily. Initially Karleigh was paralyzed and could not eat, walk or even sit up on her own. Despite many different medications, she recovered only a bit, but had at times self-injurious dystonia.
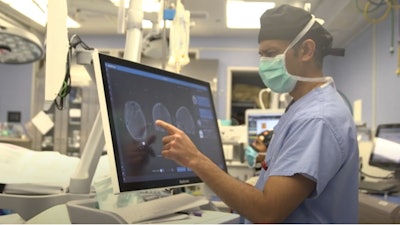
As a result, her care team at both Oklahoma Children’s Hospital and Bethany Children's explored other treatment options. Together, they decided she was a good candidate for a new procedure that would advance her care. “This marked the global debut of using a robot from our operating rooms to perform DBS in a child, setting a precedent not only in Oklahoma but also across the United States and worldwide,” said Oklahoma Children’s Hospital pediatric neurosurgeon Dr. Andrew Jea, M.D.
Following her groundbreaking surgery at Oklahoma Children’s Hospital, Karleigh’s postoperative care was seamlessly continued at Bethany Children’s Health Center, an innovative leader in the field of pediatric rehabilitation and 24-hour complex care and the only inpatient pediatric rehabilitation facility in Oklahoma.
“It’s exciting that we’re on the leading edge of what’s happening in the world of deep brain stimulation, as well as robotics,” said Dr. Amber Stocco, M.D., pediatric neurologist and medical director of Child & Adolescent Neurology at Bethany Children’s Health Center. “We are thrilled to have achieved this milestone. Our young patient is already showing promising results, and we hope this procedure will pave the way for more pediatric DBS cases worldwide.”
When the neurostimulator was activated after the procedure, Karleigh was able to lower and relax her arms within minutes, something she was unable to do prior. Her movements are becoming more controllable, and her verbalization has shown improvement as well. “Her arms used to lock up to the point we would put socks on her hands because she would scratch her neck,” said Karleigh’s mother, Trisha Fry. “There’s definitely been some improvements, even from the moment they turned it on. She is even using her voice a little bit more, and we can make out some of her words. I think she’s going to have a great future for sure.”
The successful world-first outlines the benefits of destination specialty and subspecialty programs that academic health systems can deploy and optimal results to improve the quality of pediatric patient care in Oklahoma and beyond.