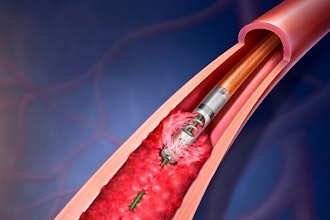
Atherosclerosis, a buildup of plaque, can lead to heart disease, artery disease, and chronic kidney disease and is traditionally treated by inserting and inflating a balloon to expand the artery. Other treatments based on lasers can remove blockages rather than simply compressing them but are used infrequently, because they have a high risk of complication and low efficacy.
Rohit Singh, of the University of Kansas, and other researchers developed a method that combines a low-power laser with ultrasound to remove arterial plaque safely and efficiently. Singh recently described preliminary results in his presentation, "A novel ultrasound-assisted laser technique to remove atherosclerotic plaques," at the 182nd Meeting of the Acoustical Society of America.
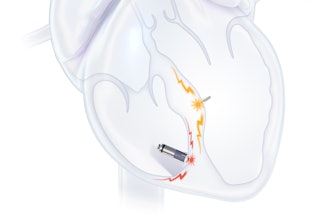
High-power laser treatments direct thermal energy to vaporize water in the artery and create a vapor bubble, which expands and collapses to break the plaque. Similarly, the technology, pioneered by Xinmai Yang, doctoral advisor for the team, uses a low-power nanosecond pulsed laser to produce microbubbles. The addition of irradiation from ultrasound causes the microbubbles to expand, collapse, and disrupt the plaque.
"In conventional laser angioplasty, a high laser power is required for the entire cavitation process, whereas in our technology, a lower laser power is only required for initiating the cavitation process," said Singh. "Overall, the combination of ultrasound and laser reduces the need for laser power and improves the efficiency of atherosclerotic plaque removal."
Because it destroys rather than compresses the plaque, the combination technique will have a lower restenosis rate, or re-narrowing of the artery, compared to balloon angioplasty or stenting. The control provided by the ultrasound and the low-power laser will lower the risk of dissection and perforation in arteries.
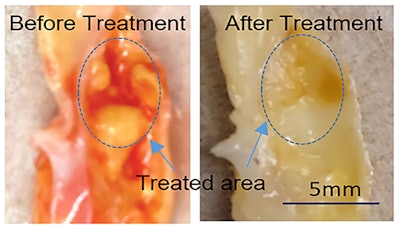
The team performed ex vivo experiments on carotid artery plaque samples and pork belly samples, and they are currently planning to perform in vivo experiments. Both the laser and ultrasound techniques are commonly used by clinicians and should be easy to teach and implement following the in vivo studies.
Combining low-power lasers and ultrasound techniques is not limited to atherosclerosis treatments. Singh and collaborators are also using the methodology for photo-mediated ultrasound therapy and ultrasound-assisted endovascular laser thrombolysis. The former can be used to remove abnormal microvessels in the eye to prevent blindness, while the latter can dissolve blood clots in veins.
Singh will expand upon these additional applications in poster sessions at the ASA meeting, with "Analysis of cavitation induced stresses on blood vessel wall during photo-mediated ultrasound therapy using finite-element based numerical models" and "Combining ultrasound and endovascular laser for thrombolysis," on May 25, 5-7 p.m. Eastern U.S.